It’s time to change the way we think about hip pain, osteoarthritis and exercise.
There is a lot of incorrect information around about hip pain, osteoarthritis and exercise. Mostly, this information is old fashioned or out of date.
Research has helped us better understand osteoarthritis and exercise. We look forward to sharing this information with you.
Review each tab to learn more about hip pain and exercise. You’ll then be ready to start your My Hip Strength program.
Hip osteoarthritis affects the whole joint. There can be changes in the cartilage, bone, ligaments and muscles of your hip. Normal day to day activities can feel more difficult than they used to. Hip pain and joint stiffness is common.
Hip osteoarthritis can usually be diagnosed by a health professional if you:
Are aged 45 or over
Have hip joint pain with activity
Have no morning hip joint stiffness OR if you have morning joint stiffness, it doesn’t last longer than 30 minutes (e.g. any joint stiffness gets better as you move and warm up in the morning)
Have no history that could suggest you have another health problem causing your joint symptoms. For example rheumatoid arthritis.
Special tests or scans are generally not needed to diagnose osteoarthritis. In most cases x-rays are not needed to diagnose osteoarthritis. Although x-rays can see osteoarthritic changes that may have affected the bones, x-rays can’t tell us if your osteoarthritis will cause you any pain. Also, x-rays can’t tell us which treatments will be most beneficial for you.
A simple way to think about it: An x-ray taken today will look the same as yesterday’s x-ray, and last week’s x-ray. In contrast, people with hip osteoarthritis know pain changes day to day or even hour to hour. We now know that the hip’s condition on x-ray does NOT equal the pain felt in the hip. Therefore, x-rays are generally not required in most cases to diagnose or help manage painful hip osteoarthritis.
Watch the video to learn more about osteoarthritis.
In the next section, we’ll discuss some more facts about osteoarthritis.
Here are references that support this information:
The Royal Australian College of General Practitioners, Guideline for the management of knee and hip osteoarthritis. 2nd edition ed, Victoria, Australia, 2018.
Bannuru RR et al., OARSI guidelines for the non-surgical management of knee, hip, and polyarticular osteoarthritis. Osteoarthritis Cartilage, 2019. 27(11): p. 1578-1589.
There is a lot of out-of-date information about osteoarthritis, which can cause lots of osteoarthritis ‘myths’ to develop and circulate.
Let’s now review the most common osteoarthritis myths.
Myth 1: Pain comes from wearing down of the cartilage.
Fact: Your joints do not wear out with everyday use. People often think osteoarthritis pain is due to ‘wear and tear’ of the joint cartilage and ‘bone rubbing on bone’. But cartilage does not have nerves. This means that cartilage changes cannot cause pain. Osteoarthritis affects the whole joint including the ligaments and muscles. These tissues can contribute to joint pain. Your mood, emotions and sleep quality can also impact the amount of pain you feel in your joint.
Myth 2: Exercise and loading the joints with osteoarthritis will cause further damage.
Fact: The opposite is true. We now know that exercise and load through the body’s joints is vital for the health of our joint tissues. This includes the cartilage, bone and muscles. The old saying of ‘use it – or lose it’ holds true. Joints need movement to keep them as healthy as possible. Avoiding exercise, like walking, to prevent the joints cartilage from ‘wearing out’ isn’t correct. In fact, regular exercise and physical activity can make many of the symptoms of osteoarthritis (such as pain) feel better!
Myth 3: Pain due to hip osteoarthritis will inevitably get worse over time.
Fact: The majority of people do not get worse. Most people remain stable. They may have bad times and good times but overall don’t continue to worsen. Some people find their symptoms even get better over time. Exercise is a great way to reduce pain and keep the hips healthy.
Myth 4: Experimental treatments will replace lost cartilage and improve joint pain.
Fact: Unfortunately, there are no quick fixes when it comes to osteoarthritis. Experimental treatments, such as stem cell injections are expensive and currently there is no good quality research showing that they work. Stem cells or platelet rich plasma injections into the joint are not currently recommended. Also, surgeries to ‘clean out the joint’ typically don’t improve joint symptoms and are not recommended for people with osteoarthritis anymore. Exercise and maintaining a healthy weight are the key recommended treatments. This is based on strong scientific evidence.
Myth 5: Joint replacement surgery is inevitable.
Fact: For most people, symptoms of osteoarthritis will generally be stable, with occasional flare-ups from time to time. While a flare will make you feel worse for a little while, the pain will usually settle down again in time. Most people’s osteoarthritis will not become severe enough to need a joint replacement. In fact, your pain may improve over time.
In the next section, we’ll discuss pain and what influences joint pain.
Here are references that support this information:
National Clinical Guideline Centre. Osteoarthritis. Osteoarthritis in over 16s: diagnosis and management. Clinical guideline NG226. Methods, evidence and recommendations. London; National Institute for Health and Care Excellence, 2022.
Kraus V et al., Effects of Physical Activity in Knee and Hip Osteoarthritis: A Systematic Umbrella Review, Medicine & Science in Sports & Exercise, 2019; 51(6).
Fransen M et al., Exercise for osteoarthritis of the hip. Cochrane Database of Systematic Reviews, 2014.
Hunter DJ et al., Osteoarthritis. The Lancet 2019; 393: 1745.
Pain is the most common symptom of hip osteoarthritis.
Learning more about the factors that can influence your hip pain can help you better manage it.
Pain is complex. Pain is not a simple matter of ‘damage leads to pain’. Increased joint pain generally does not mean that you have damaged your joint. It used to be thought that pain was just a simple message from your osteoarthritic joint straight to the brain. However, lots of research has shown that pain is much more complex than that, and that the brain can change how you interpret messages of pain. There are a range of different factors that influence why and how you feel pain, including;
the sensations from your hip joint and surrounding muscle and tissues
your mood, anxiety and stress levels
your fatigue levels and/or quality of sleep
your thoughts, worries and fears about pain
sometimes just focussing too much on the pain can make it seem worse.
It’s the brain and nervous system’s job to make sense of all these factors and decide if you feel pain and how much. Think of the brain like a volume dial. The brain interprets all the factors that influence your pain. The brain then decides to turn the pain level up or down. For example, when you feel stress or anxiety the pain volume can turn up. When you do something fun that distracts you, the pain volume can turn down.
If you’ve had pain for a long time your pain system becomes overly protective. This means things that didn’t previously hurt now do. It makes sense. If you’re in pain, you want to avoid activity. But being less active can make your pain worse over time. Inactivity causes muscle weakness and loss of cardiovascular fitness. You can gain weight. Your mood and sleep problems can get worse. All these things can make your pain worse and make you avoid activity even more.
Excitingly, pain scientists have discovered that everyone can ‘retrain’ their pain system. If you change how you think about and respond to pain, you can take more control of your pain. You can start retraining your pain system by slowly increasing how much you move and how active you are.
Watch the video below to learn more. In the video, Australian Pain Scientist Professor Moseley describes new discoveries about persistent pain. He also talks about the importance of exercise and movement in pain management.
The best way to break the cycle of pain and less activity is:
Strengthen your hip muscles: Strong muscles can keep the hip joint healthy and reduce pain. My Hip Strength will help you get started.
Stay as active as you can: Being active can keep the hip joints healthy and reduce pain. It’s also a good idea for weight management and overall health. My Hip Activity has tips to help you become more active.
In the next section, we’ll discuss hip pain and hip osteoarthritis treatments.
Here is a reference that supports this information:
Butler DS, et al., . Explain Pain: Noigroup Publications, 2013.
Hip OA can be managed successfully.
The most beneficial treatments for ALL people with hip OA are exercise and physical activity. In addition to these treatments pain-relieving medication may be suitable for some people. In some cases, where symptoms are severe and other treatments are not helping, joint surgery may be a suitable option.
Exercise. Regular exercise has many benefits for people with hip OA. It helps reduce symptoms (e.g. pain, stiffness). It improves hip mobility and muscle strength. It improves sleep quality and mood. But, starting exercise with a sore hip can be hard. That’s why My Hip Exercise was designed – to help people with painful hips start exercise safely.
Some other ways to manage hip pain include:
Education. Learn about hip OA. Read all the information provided in My Hip Education to better understand hip pain and exercise. You might like to visit other websites for more information. See the list at the bottom of this page.
Weight management. Controlling weight (if needed) is important for general health. Although, currently there isn’t enough research to know if weight loss reduces hip pain. If you’d like to explore weight loss, speak with your doctor for advice on safe and effective weight loss strategies.
Assistive walking devices. Canes (e.g., walking sticks), crutches and walkers can help you stand more upright, reduce pressure on your joint, improve balance and may help with pain. They are also helpful to reduce falls risk. They can be purchased or rented from physiotherapy clinics, pharmacies, or online retailers.
Medication. Pain-relieving medication can help during times of more severe pain. Speak with your doctor to find out what medication might work for you.
Relaxation & pain coping techniques. Techniques to try include meditation, progressive muscle relaxation and pleasant imagery. They can help manage pain. They can also help with emotions. Worry, fear, anxiety, even anger are all common things to feel when you’ve had pain for a long time.
Surgery. If you have tried other treatments including exercise and weight management (if appropriate) OR if your hip OA is advanced OR if symptoms can no longer be tolerated, surgery might be an option. The hip joint can be replaced with an artificial joint.
Watch the video to learn more about recommended osteoarthritis treatments.
If you would like to learn even more about osteoarthritis and strategies to manage pain, you might find the two websites below useful. They are resources that have been developed by the My Hip Exercise research team.
Taking Control of Your Hip and Knee Osteoarthritis is a four-week online course on FutureLearn. Learn about hip and knee osteoarthritis and strategies to manage pain, including exercise, healthy weight, and pain relief.
painTRAINER is an interactive, online tool that teaches you effective strategies to manage your pain. The painTRAINER program is made up of 8 sessions, each lasting about 30-45 minutes.
In the next section, we’ll discuss more about exercise as a treatment for hip OA.
Here are references that support this information:
The Royal Australian College of General Practitioners, Guideline for the management of knee and hip osteoarthritis. 2nd edition ed, Victoria, Australia, 2018.
Bannuru RR et al., OARSI guidelines for the non-surgical management of knee, hip, and polyarticular osteoarthritis. Osteoarthritis Cartilage, 2019. 27(11): p. 1578-1589.
National Clinical Guideline Centre. Osteoarthritis. Osteoarthritis in over 16s: diagnosis and management. Clinical guideline NG226. Methods, evidence and recommendations. London; National Institute for Health and Care Excellence, 2022.
Exercise is an important treatment for hip osteoarthritis.
Sadly, many people with painful hips are not exercising. A lot of people with painful hips think they shouldn’t exercise. But, exercise is a vital part of managing hip pain, even very painful hips.
Regular exercise:
![]() keeps joints healthy and moving
keeps joints healthy and moving
![]() maintains fitness
maintains fitness
![]() improves mood
improves mood
![]() maintains weight
maintains weight
![]() reduces the risk of other health conditions that can make managing hip pain harder (obesity, heart conditions, diabetes)
reduces the risk of other health conditions that can make managing hip pain harder (obesity, heart conditions, diabetes)
![]() can lower feelings of social isolation if done with other people
can lower feelings of social isolation if done with other people
Also, regular exercise can prevent or reduce the need for pain relieving medication. In fact, scientific research has shown the benefits of exercise on pain are similar to the effects achieved with pain relieving medications like paracetamol and non steroidal anti inflammatory drugs (NSAIDs) – but exercise doesn’t have the risks or side effects of medications!
Scientific evidence has also shown exercise can help people with osteoarthritis avoid or delay the need for joint replacement surgery. In fact, exercise can reduce the need for a hip replacement by up to 68%!
Everyone, even people with painful hips, should be exercising.
Strength exercise and general physical activity are recommended for all people with hip osteoarthritis.
Strength exercise:
All people with hip osteoarthritis should do some type of leg strengthening exercise. Regular strength exercise makes the muscles around your hip strong and supportive. Over time strength exercise can reduce pain and help you be more active. It’s recommended to do 3 sessions each week to see benefits. My Hip Strength contains your recommended 6-month hip strength program to get you started.
General physical activity:
For hip and general health, people should spend some time on most days being physically active. It’s recommended everyone do at least 150-300 minutes of moderate intensity (e.g. brisk walking, doubles tennis) aerobic physical activity per week. Moderate activity means you feel like you’re putting in some effort and not just cruising along being gentle. But, if moderate activity is too difficult or causes discomfort, light activity is still beneficial. You also don’t need to do 20-60 minutes of activity all at once. Bouts of activity 10 minutes at a time works too! My Hip Activity contains useful information to help you increase your general physical activity in the next 6-months and beyond.
Watch the video to learn more about exercising with osteoarthritis.
In the next section, we’ll discuss common concerns people with hip osteoarthritis have about exercising.
Here is a reference that supports this information:
Kraus V et al., Effects of Physical Activity in Knee and Hip Osteoarthritis: A Systematic Umbrella Review, Medicine & Science in Sports & Exercise, 2019; 51(6).
Fransen M et al., Exercise for osteoarthritis of the hip. Cochrane Database of Systematic Reviews, 2014.
World Health Organization. WHO guidelines on physical activity and sedentary behaviour. Geneva: World Health Organization; 2020.
Although exercise is an important part of managing osteoarthritis, many people with hip pain feel nervous about starting regular exercise. Let’s discuss three common concerns people with hip osteoarthritis have about exercise.
Concern 1: “Exercise will further damage my joint”
Response: The opposite is true- research shows that “loading” joints, for example when you exercise, is important for the health of a joint’s cartilage. Think of exercise as a joint lubricant. Many people avoid using their painful joint for fear of making it worse. But, when you don’t move your joints, they become stiffer. The muscles around the joint become weaker and less supportive. Over time, this can lead to even more pain and stiffness. The old saying of ‘use it – or lose it’ holds true. Our joints need movement and exercise to keep them as healthy as possible.
Concern 2: “Last time I exercised my joint pain got worse”
Response: It’s common to feel pain in your muscles or joint during or straight after exercise. Even people who don’t have osteoarthritis feel this too. Research suggests that pain flares (an increase in joint pain) are acceptable and safe, as long as pain returns to baseline levels within about 24 hours after exercise. Remember that pain isn’t an accurate measure of what is happening inside the joint. But, if you do find that pain is limiting your ability to stick to exercise, or your pain is aggravated for more than 24 hours after exercise, it might be time to seek professional help. For example, a physiotherapist is a trained exercise expert. They can tailor a program to your needs and abilities.
Concern 3: “Exercise is a waste of time. I’ve exercised before, it didn’t make a difference”
Response: Don’t be worried if exercise doesn’t result in immediate pain relief. It takes time and commitment to see benefits. It can take up to 12 weeks to see real changes in your symptoms. For example, research shows that it can take 4-12 weeks to start to see changes in your muscle strength after doing consistent strength training. It’s also important to keep challenging yourself and progress your exercise routine when it becomes too easy. This way you keep improving. You might also find some types of exercise work better for you than others. So, another thing to consider is trying a different type of exercise. You’ll find a range of ideas in the next section ‘What physical activity and exercise is suitable for people with osteoarthritis?’. If you’re still having trouble seeing benefits from exercise, it might be time to seek professional help. A physiotherapist can help you progress your exercises, so you keep seeing benefits over time.
Watch the video to learn more about the safety of exercise for people with osteoarthritis.
In the next section, we’ll discuss how to get started with your My Hip Exercise program.
Here are references that support this information:
Kraus V et al., Effects of Physical Activity in Knee and Hip Osteoarthritis: A Systematic Umbrella Review, Medicine & Science in Sports & Exercise, 2019; 51(6).
Fransen M et al., Exercise for osteoarthritis of the hip. Cochrane Database of Systematic Reviews, 2014.
Hunter DJ et al,.. Osteoarthritis. The Lancet 2019; 393: 1745.
Start your My Hip Exercise program this week.
How to get started:
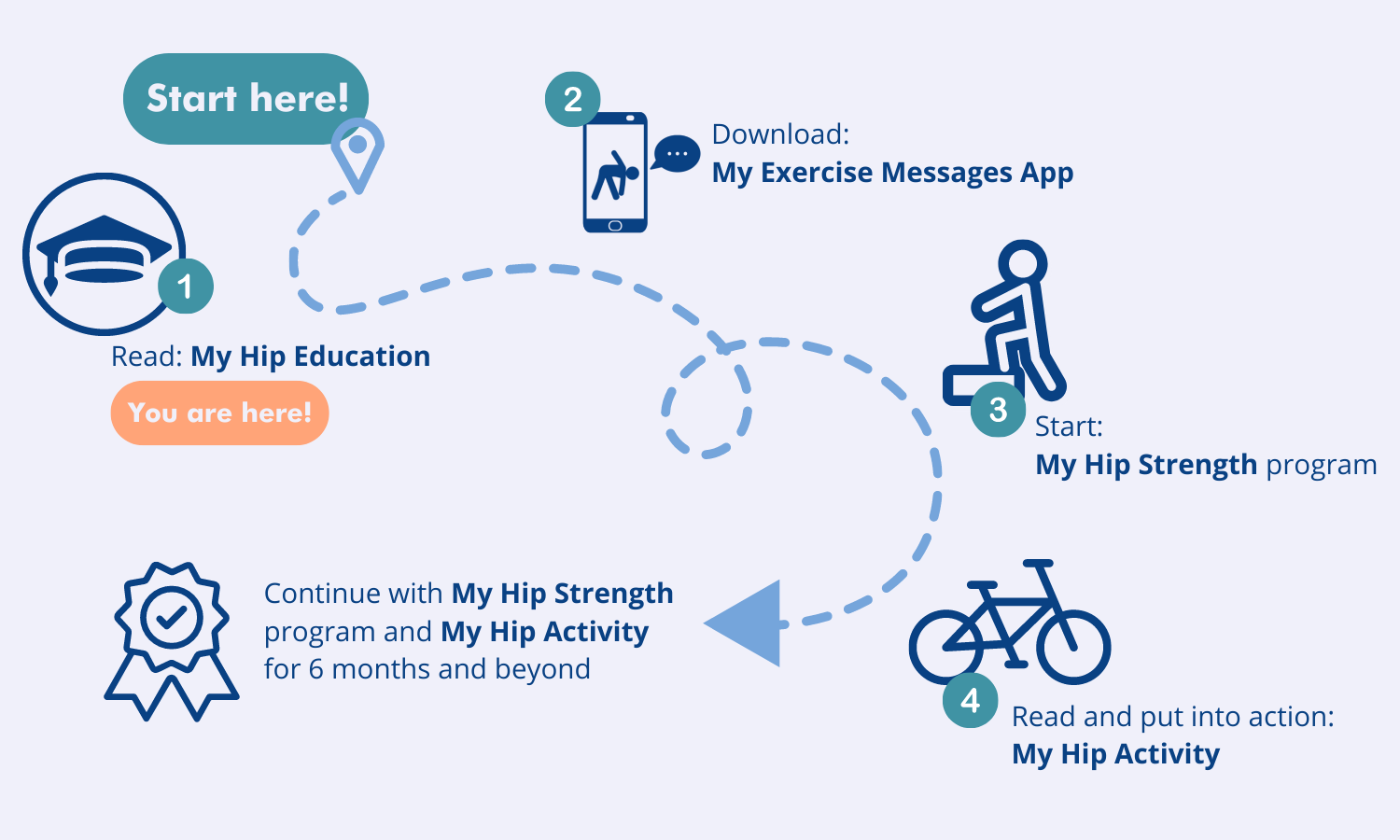
After reading the My Hip Education information it’s time to start your exercise program.
STEP 1
Go to My Exercise Messages App. You’ll find the tab at the top of this page, or there’s a button below.
Follow the instructions to download and set up the app on your mobile phone. Please set up the app this week. You are asked to use the app to record your My Hip Strength exercise sessions each week.
STEP 2
Go to My Hip Strength. You’ll find the link at the top of the page.
Go to ‘Introduction’. Read the information provided in all the tabs.
Go to ‘Program 1’. Follow the instructions and start your 5 hip exercises this week.
STEP 3
Go to My Hip Activity. You’ll find the link at the top of the page.
This section will help guide you in how to start gradually increasing your overall activity levels.